Magnetic Resonance Imaging
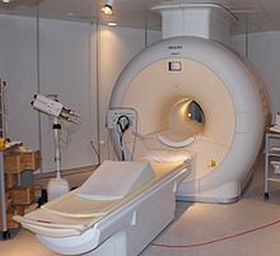
Magnetic resonance imaging (MRI), nuclear magnetic resonance imaging (NMRI), or magnetic resonance tomography (MRT) is a medical imaging technique used in radiology to visualize internal structures of the body in detail. MRI makes use of the property of nuclear magnetic resonance (NMR) to image nuclei of atoms inside the body. MRI can create more detailed images of the human body than are possible with X-rays.
An MRI scanner is a device in which the patient lies within a large, powerful magnet where the magnetic field is used to align the magnetization of some atomic nuclei in the body, and radio frequency magnetic fields are applied to systematically alter the alignment of this magnetization. This causes the nuclei to produce a rotating magnetic field detectable by the scanner—and this information is recorded to construct an image of the scanned area of the body. Magnetic field gradients cause nuclei at different locations to precess at different speeds, which allows spatial information to be recovered using Fourier analysis of the measured signal. By using gradients in different directions, 2D images or 3D volumes can be obtained in any arbitrary orientation.
MRI provides good contrast between the different soft tissues of the body, which makes it especially useful in imaging the brain, muscles, the heart, and cancers compared with other medical imaging techniques such as computed tomography (CT) or X-rays. Unlike CT scans or traditional X-rays, MRI does not use ionizing radiation.
An MRI scanner is a device in which the patient lies within a large, powerful magnet where the magnetic field is used to align the magnetization of some atomic nuclei in the body, and radio frequency magnetic fields are applied to systematically alter the alignment of this magnetization. This causes the nuclei to produce a rotating magnetic field detectable by the scanner—and this information is recorded to construct an image of the scanned area of the body. Magnetic field gradients cause nuclei at different locations to precess at different speeds, which allows spatial information to be recovered using Fourier analysis of the measured signal. By using gradients in different directions, 2D images or 3D volumes can be obtained in any arbitrary orientation.
MRI provides good contrast between the different soft tissues of the body, which makes it especially useful in imaging the brain, muscles, the heart, and cancers compared with other medical imaging techniques such as computed tomography (CT) or X-rays. Unlike CT scans or traditional X-rays, MRI does not use ionizing radiation.
How MRI Works

MRI machines make use of the fact that body tissue contains lots of water, and hence protons (1H nuclei), which get aligned in a large magnetic field. Each water molecule has two hydrogen nuclei or protons. When a person is inside the powerful magnetic field of the scanner, the average magnetic moment of many protons becomes aligned with the direction of the field. A radio frequency current is briefly turned on, producing a varying electromagnetic field. This electromagnetic field has just the right frequency, known as the resonance frequency, to be absorbed and flip the spin of the protons in the magnetic field. After the electromagnetic field is turned off, the spins of the protons return to thermodynamic equilibrium and the bulk magnetization becomes re-aligned with the static magnetic field. During this relaxation, a radio frequency signal (electromagnetic radiation in the RF range) is generated, which can be measured with receiver coils.
Information about the origin of the signal in 3D space can be learned by applying additional magnetic fields during the scan. These additional magnetic fields can be used to generate detectable signal only from specific locations in the body (spatial excitation) and/or to make magnetization at different spatial locations precess at different frequencies, which enables k-space encoding of spatial information. The 3D images obtained in MRI can be rotated along arbitrary orientations and manipulated by the doctor to be better able to detect tiny changes of structures within the body. These fields, generated by passing electric currents through gradient coils, make the magnetic field strength vary depending on the position within the magnet. Because this makes the frequency of the released radio signal also dependent on its origin in a predictable manner, the distribution of protons in the body can be mathematically recovered from the signal, typically by the use of inverse Fourier transform.
Protons in different tissues return to their equilibrium state at different relaxation rates. Different tissue variables, including spin density, T1 and T2 relaxation times, and flow and spectral shifts, can be used to construct images. By changing the settings on the scanner, this effect is used to create contrast between different types of body tissue or between other properties, as in fMRI and diffusion MRI.
MRI is used to image every part of the body, and is particularly useful for tissues with many hydrogen nuclei and little density contrast, such as the brain, muscle, connective tissue and most tumors.
Information about the origin of the signal in 3D space can be learned by applying additional magnetic fields during the scan. These additional magnetic fields can be used to generate detectable signal only from specific locations in the body (spatial excitation) and/or to make magnetization at different spatial locations precess at different frequencies, which enables k-space encoding of spatial information. The 3D images obtained in MRI can be rotated along arbitrary orientations and manipulated by the doctor to be better able to detect tiny changes of structures within the body. These fields, generated by passing electric currents through gradient coils, make the magnetic field strength vary depending on the position within the magnet. Because this makes the frequency of the released radio signal also dependent on its origin in a predictable manner, the distribution of protons in the body can be mathematically recovered from the signal, typically by the use of inverse Fourier transform.
Protons in different tissues return to their equilibrium state at different relaxation rates. Different tissue variables, including spin density, T1 and T2 relaxation times, and flow and spectral shifts, can be used to construct images. By changing the settings on the scanner, this effect is used to create contrast between different types of body tissue or between other properties, as in fMRI and diffusion MRI.
MRI is used to image every part of the body, and is particularly useful for tissues with many hydrogen nuclei and little density contrast, such as the brain, muscle, connective tissue and most tumors.
Magnetic field
MRI scans require a magnetic field with two properties, uniform field density and strength. The magnetic field cannot vary more than 1/10,000 of 1% and field strength ranges (depending on the scanner) from 0.2 to 3 teslas in strength in currently clinically used scanners, with research scanners investigating higher field strengths such as seven teslas. The lower field strengths can be achieved with permanent magnets, which are often used in "open" MRI scanners for claustrophobic patients. Higher field strengths can be achieved only with superconducting magnets. An MRI with a 3.0 tesla strength magnet may be referred to as a "3-T MRI" or "3-tesla MRI"
Since the gradient coils are within the bore of the scanner, there are large forces between them and the main field coils, producing most of the noise that is heard during operation. Without efforts to damp this noise, it can approach 130 decibels (dB) with strong fields (see also the subsection on acoustic noise).
Contrast agents and implants
MRI contrast agents may be injected intravenously to enhance the appearance of blood vessels, tumors or inflammation. Contrast agents may also be directly injected into a joint in the case of arthrograms: MRI images of joints. Unlike CT, MRI uses no ionizing radiation and is generally a very safe procedure. Nonetheless the strong magnetic fields and radio pulses can affect metal implants, including cochlear implants and cardiac pacemakers. There are many electronically activated devices that have approval from the US FDA to permit MRI procedures in patients under highly specific MRI conditions (see www.MRIsafety.com). In the case of cochlear implants, the US FDA has approved some implants for MRI compatibility. In the case of cardiac pacemakers, the results can sometimes be lethal,so patients with such implants are generally not eligible for MRI.
Prepolarized MRI
In 2001, a research team at Stanford invented a new technique which came to be called "Prepolarized MRI" or PMRI. The team demonstrated that the magnets do not have to be both uniform and strong. Rather, two magnets can be used together, where one is strong and the other one is uniform.
The first magnet in a PMRI scanner is strong, but not uniform. This magnet creates a very strong magnetic field which varies in uniformity by as much as 40%. This is the "prepolarize" component. A second much weaker (requiring only the electric power necessary to run two hairdryers) but far more precise magnet then creates a homogeneous magnetic field. These two magnets can be ordinary copper wound magnets, greatly lowering the cost of an MRI scanner. Because the magnetic field is "tuned" by the second magnet, a PMRI scan can be obtained immediately adjacent to a metal prosthetic, unlike an MRI scan.
History
In 1952, Herman Carr produced a one-dimensional MRI image as reported in his Harvard PhD thesis. In the Soviet Union, Vladislav Ivanov filed (in 1960) a document with the USSR State Committee for Inventions and Discovery at Leningrad for a Magnetic Resonance Imaging device, although this was not approved until the 1970s.
Raymond Damadian's "Apparatus and method for detecting cancer in tissue." In a 1971 paper in the journal Science,Raymond Damadian, an Armenian-American physician, scientist, and professor at the Downstate Medical Center State University of New York (SUNY), reported that tumors and normal tissue can be distinguished in vivo by nuclear magnetic resonance ("NMR"). He suggested that these differences could be used to diagnose cancer, though later research would find that these differences, while real, are too variable for diagnostic purposes. Damadian's initial methods were flawed for practical use, relying on a point-by-point scan of the entire body and using relaxation rates, which turned out not to be an effective indicator of cancerous tissue. While researching the analytical properties of magnetic resonance, Damadian created the world's first magnetic resonance imaging machine in 1972. He filed the first patent for an MRI machine, U.S. patent #3,789,832 on March 17, 1972, which was later issued to him on February 5, 1974.
The National Science Foundation notes, "The patent included the idea of using NMR to 'scan' the human body to locate cancerous tissue."However, it did not describe a method for generating pictures from such a scan or precisely how such a scan might be done. Meanwhile, Paul Lauterbur expanded on Carr's technique and developed a way to generate the first MRI images, in 2D and 3D, using gradients. In 1973, Lauterbur published the first nuclear magnetic resonance image and the first cross-sectional image of a living mouse in January 1974. In the late 1970s, Peter Mansfield, a physicist and professor at the University of Nottingham, England, developed a mathematical technique that would allow scans to take seconds rather than hours and produce clearer images than Lauterbur had. Damadian, along with Larry Minkoff and Michael Goldsmith, performed the first MRI body scan of a human being on July 3, 1977,studies which they published in 1977.and in 1979 Richard S. Likes filed patent *.
In 1980 Paul Bottomley joined the GE Research Center in Schenectady, NY, and his team ordered the highest field-strength magnet then available — a 1.5T system — and built the first high-field and overcame problems of coil design, RF penetration and signal-to-noise ratio to build the first whole-body MRI/MRS scanner. The results translated into the highly successful 1.5T MRI product-line, with over 20,000 systems in use today. Bottomley performed the first localized MRS in the human heart and brain. After starting a collaboration on heart applications with Robert Weiss at Johns Hopkins, Bottomley returned to the university in 1994 as Russell Morgan Professor and director of the MR Research Division. Although MRI is most commonly performed at 1.5 T, higher fields such as 3T are gaining more popularity because of their increased sensitivity and resolution. In research laboratories, human studies have been performed at up to 9.4 T and animal studies have been performed at up to 21.1T.
Applications
In clinical practice, MRI is used to distinguish pathologic tissue (such as a brain tumor) from normal tissue. One advantage of an MRI scan is that it is harmless to the patient. It uses strong magnetic fields and non-ionizing electromagnetic fields in the radio frequency range, unlike CT scans and traditional X-rays, which both use ionizing radiation.
While CT provides good spatial resolution (the ability to distinguish two separate structures at a small distance from each other), MRI provides comparable resolution with far better contrast resolution (the ability to distinguish the differences between two similar but not identical tissues). The basis of this ability is the complex library of pulse sequences that the modern medical MRI scanner includes, each of which is optimized to provide image contrast based on the chemical sensitivity of MRI.
Effects of TR and TE on MR signal. For example, with particular values of the echo time (TE) and the repetition time (TR), which are basic parameters of image acquisition, a sequence takes on the property of T2-weighting. On a T2-weighted scan, water- and fluid-containing tissues are bright (most modern T2 sequences are actually fast T2 sequences) and fat-containing tissues are dark. The reverse is true for T1-weighted images. Damaged tissue tends to develop edema, which makes a T2-weighted sequence sensitive for pathology, and generally able to distinguish pathologic tissue from normal tissue. With the addition of an additional radio frequency pulse and additional manipulation of the magnetic gradients, a T2-weighted sequence can be converted to a FLAIR sequence, in which free water is now dark, but edematous tissues remain bright. This sequence in particular is currently the most sensitive way to evaluate the brain for demyelinating diseases, such as multiple sclerosis.
The typical MRI examination consists of 5–20 sequences, each of which is chosen to provide a particular type of information about the subject tissues. This information is then synthesized by the interpreting physician.
MRI scans require a magnetic field with two properties, uniform field density and strength. The magnetic field cannot vary more than 1/10,000 of 1% and field strength ranges (depending on the scanner) from 0.2 to 3 teslas in strength in currently clinically used scanners, with research scanners investigating higher field strengths such as seven teslas. The lower field strengths can be achieved with permanent magnets, which are often used in "open" MRI scanners for claustrophobic patients. Higher field strengths can be achieved only with superconducting magnets. An MRI with a 3.0 tesla strength magnet may be referred to as a "3-T MRI" or "3-tesla MRI"
Since the gradient coils are within the bore of the scanner, there are large forces between them and the main field coils, producing most of the noise that is heard during operation. Without efforts to damp this noise, it can approach 130 decibels (dB) with strong fields (see also the subsection on acoustic noise).
Contrast agents and implants
MRI contrast agents may be injected intravenously to enhance the appearance of blood vessels, tumors or inflammation. Contrast agents may also be directly injected into a joint in the case of arthrograms: MRI images of joints. Unlike CT, MRI uses no ionizing radiation and is generally a very safe procedure. Nonetheless the strong magnetic fields and radio pulses can affect metal implants, including cochlear implants and cardiac pacemakers. There are many electronically activated devices that have approval from the US FDA to permit MRI procedures in patients under highly specific MRI conditions (see www.MRIsafety.com). In the case of cochlear implants, the US FDA has approved some implants for MRI compatibility. In the case of cardiac pacemakers, the results can sometimes be lethal,so patients with such implants are generally not eligible for MRI.
Prepolarized MRI
In 2001, a research team at Stanford invented a new technique which came to be called "Prepolarized MRI" or PMRI. The team demonstrated that the magnets do not have to be both uniform and strong. Rather, two magnets can be used together, where one is strong and the other one is uniform.
The first magnet in a PMRI scanner is strong, but not uniform. This magnet creates a very strong magnetic field which varies in uniformity by as much as 40%. This is the "prepolarize" component. A second much weaker (requiring only the electric power necessary to run two hairdryers) but far more precise magnet then creates a homogeneous magnetic field. These two magnets can be ordinary copper wound magnets, greatly lowering the cost of an MRI scanner. Because the magnetic field is "tuned" by the second magnet, a PMRI scan can be obtained immediately adjacent to a metal prosthetic, unlike an MRI scan.
History
In 1952, Herman Carr produced a one-dimensional MRI image as reported in his Harvard PhD thesis. In the Soviet Union, Vladislav Ivanov filed (in 1960) a document with the USSR State Committee for Inventions and Discovery at Leningrad for a Magnetic Resonance Imaging device, although this was not approved until the 1970s.
Raymond Damadian's "Apparatus and method for detecting cancer in tissue." In a 1971 paper in the journal Science,Raymond Damadian, an Armenian-American physician, scientist, and professor at the Downstate Medical Center State University of New York (SUNY), reported that tumors and normal tissue can be distinguished in vivo by nuclear magnetic resonance ("NMR"). He suggested that these differences could be used to diagnose cancer, though later research would find that these differences, while real, are too variable for diagnostic purposes. Damadian's initial methods were flawed for practical use, relying on a point-by-point scan of the entire body and using relaxation rates, which turned out not to be an effective indicator of cancerous tissue. While researching the analytical properties of magnetic resonance, Damadian created the world's first magnetic resonance imaging machine in 1972. He filed the first patent for an MRI machine, U.S. patent #3,789,832 on March 17, 1972, which was later issued to him on February 5, 1974.
The National Science Foundation notes, "The patent included the idea of using NMR to 'scan' the human body to locate cancerous tissue."However, it did not describe a method for generating pictures from such a scan or precisely how such a scan might be done. Meanwhile, Paul Lauterbur expanded on Carr's technique and developed a way to generate the first MRI images, in 2D and 3D, using gradients. In 1973, Lauterbur published the first nuclear magnetic resonance image and the first cross-sectional image of a living mouse in January 1974. In the late 1970s, Peter Mansfield, a physicist and professor at the University of Nottingham, England, developed a mathematical technique that would allow scans to take seconds rather than hours and produce clearer images than Lauterbur had. Damadian, along with Larry Minkoff and Michael Goldsmith, performed the first MRI body scan of a human being on July 3, 1977,studies which they published in 1977.and in 1979 Richard S. Likes filed patent *.
In 1980 Paul Bottomley joined the GE Research Center in Schenectady, NY, and his team ordered the highest field-strength magnet then available — a 1.5T system — and built the first high-field and overcame problems of coil design, RF penetration and signal-to-noise ratio to build the first whole-body MRI/MRS scanner. The results translated into the highly successful 1.5T MRI product-line, with over 20,000 systems in use today. Bottomley performed the first localized MRS in the human heart and brain. After starting a collaboration on heart applications with Robert Weiss at Johns Hopkins, Bottomley returned to the university in 1994 as Russell Morgan Professor and director of the MR Research Division. Although MRI is most commonly performed at 1.5 T, higher fields such as 3T are gaining more popularity because of their increased sensitivity and resolution. In research laboratories, human studies have been performed at up to 9.4 T and animal studies have been performed at up to 21.1T.
Applications
In clinical practice, MRI is used to distinguish pathologic tissue (such as a brain tumor) from normal tissue. One advantage of an MRI scan is that it is harmless to the patient. It uses strong magnetic fields and non-ionizing electromagnetic fields in the radio frequency range, unlike CT scans and traditional X-rays, which both use ionizing radiation.
While CT provides good spatial resolution (the ability to distinguish two separate structures at a small distance from each other), MRI provides comparable resolution with far better contrast resolution (the ability to distinguish the differences between two similar but not identical tissues). The basis of this ability is the complex library of pulse sequences that the modern medical MRI scanner includes, each of which is optimized to provide image contrast based on the chemical sensitivity of MRI.
Effects of TR and TE on MR signal. For example, with particular values of the echo time (TE) and the repetition time (TR), which are basic parameters of image acquisition, a sequence takes on the property of T2-weighting. On a T2-weighted scan, water- and fluid-containing tissues are bright (most modern T2 sequences are actually fast T2 sequences) and fat-containing tissues are dark. The reverse is true for T1-weighted images. Damaged tissue tends to develop edema, which makes a T2-weighted sequence sensitive for pathology, and generally able to distinguish pathologic tissue from normal tissue. With the addition of an additional radio frequency pulse and additional manipulation of the magnetic gradients, a T2-weighted sequence can be converted to a FLAIR sequence, in which free water is now dark, but edematous tissues remain bright. This sequence in particular is currently the most sensitive way to evaluate the brain for demyelinating diseases, such as multiple sclerosis.
The typical MRI examination consists of 5–20 sequences, each of which is chosen to provide a particular type of information about the subject tissues. This information is then synthesized by the interpreting physician.

