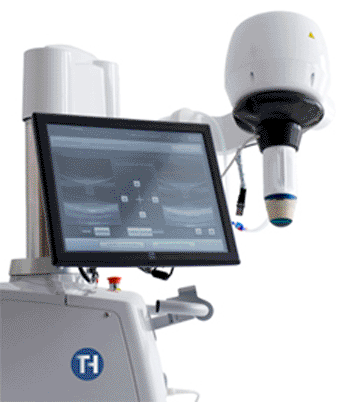
A new noninvasive therapeutic application using ultrasound-guided, high-intensity focused ultrasound (HIFU) is currently being employed for a specifically localized ablation with no skin damage. The ultrasound waves are focused on a small area where the rise in temperature leads to tissue necrosis. This precision avoids injuring healthy tissues around the lesion. The echotherapy is a technique that enables clinicians to visualize and simultaneously treat a tumor such as fibroadenoma with no incision or scar.
|
A medical imaging facility in California has implemented an effective program focused on radiation dose reduction, slashing exposure to radiation by up to 90% in some cases.
A Canadian heart institute is putting into play what could become a transformation in medical imaging in Canada as it presented findings in radiation reduction for the diagnosis of cardiovascular disease.
As a result of an initiative that combines optimizing test protocols, state-of-the art equipment, and high-tech software, two-thirds of the Ottawa Heart Institutes (UOHI; Ottawa, Ontario, Canada) nuclear cardiology patients are currently receiving half the radiation dosage that they would normally get. Radiation reduction techniques have been accomplished across all kinds of radiation-based cardiac imaging--computed tomography (CT), nuclear imaging, and positron emission tomography (PET). The Heart Institute is one of only a one of a couple of centers in Canada with the in-house expertise to assess and clinically apply these latest developments across these technologies. The American Society for Nuclear Cardiology has challenged the nuclear cardiology community to reduce radiation exposure below 9 millisieverts (mSv) by 2014. The techniques being employed at the Heart Institute regularly reduce exposure to 5 mSv, and frequently much less, putting UOHI well ahead of the game. This figure has not bottomed out, as efforts will continue to minimize radiation wherever possible. “Our clinicians are taking a much more critical look at who they are testing with radioactive methods and making decisions based upon risk and necessity which will only expose patients to radiation who truly need the test,” said Dr. Benjamin Chow, codirector of cardiac radiology at the University of Ottawa Heart Institute. These responsible practices, along with a judicious use of technology, could revolutionize cardiac imaging in Canada.” The payback for this effort include reduced radiation dosages for patients, greater flexibility for customizing modalities for patients, and, in some instances, a decreased need placed on radioisotopes. For example, for younger patients, radiation exposure presents greater risks because they have more years in which cancer could develop. So lessening their dosage is a high priority. In the case of older patients whose lives may be threatened by an immediate cardiac problem condition, the advantages would overshadow the small risk of developing cancer later in life. UOHI also uses a combination of effective applications that facilitate a better diagnosis of cardiovascular problems. The cadmium-zinc-telluride camera system used for nuclear imaging is a significant development and it was implemented by Dr. Glenn Wells, medical physicist in nuclear cardiology. The Heart Institute was one of the first centers in the world with this technology in 2009, and it had a major impact on reducing radiation in perfusion single emission computed tomography (SPECT) scans, the most typical cardiac imaging modality. The introduction of PET imaging in the late 1990s, which provides much more detailed imagery with much lower levels of injected isotopes, has also had an impact on reducing radiation exposure. The use of these cameras in Canada is still uncommon but increasing. Software is another critical part of imaging, transforming the scanner data into coherent two- or even three-dimensional (3D) images of what is seen in a patient’s body. The Heart Institute has helped commercial developers evaluate and enhance new, sophisticated software packages for both PET and SPECT scanners that maintain image quality while using less radioactive isotopes. Radiation has become a concern for both medical professionals and patients; however, frequently people do not realize the considerable advantages of very effective diagnostic imaging modalities that may require very low amounts of medical radiation. “Careful and appropriate selection of the right test for the right patient balancing benefit and risk enables optimal patient care,” said Dr. Terrence Ruddy, director of nuclear cardiology, University of Ottawa Heart Institute. An N-Methyl-D-aspartate receptor antagonist called memantin, which is usually prescribed to Alzheimer’s disease (AD) patients, has been shown to slow cognitive decline in brain cancer patients who receive whole brain radiation therapy (WBRT).
The findings were presented October 31, 2012, at the American Society for Radiation Oncology’s (ASTRO’s) 54th annual meeting, held October 2012 in Boston (MA, USA). The phase III trial assessed the possible protective effects of memantine on cognitive function in 508 patients with brain tumors who received WBRT between March 2008 and July 2010. In addition to cognitive function, the study examined the length of time before suffering cognitive decline, overall survival (OS), and progression-free survival (PFS). Patients received WBRT of 37.5 Gy in 15 fractions and they were randomized to receive placebo or a 20-mg dose of memantine a day within three days of initiating radiotherapy for 24 weeks. Results demonstrate that memantine delays cognitive decline of recognition memory, global and executive function, and processing speed regions of the brain. Patients in the memantine group experienced a 17% relative reduction in cognitive decline at 24 weeks compared to those in the placebo group. Patients’ cognitive function as assessed utilizing the Controlled Oral Word Association test at 8 and 16 weeks and the Trail Making Test Part A at 24 weeks also revealed fewer patients in the memantine group experienced decline. Patients were also evaluated at 24 weeks with the Hopkins Verbal Learning Test-Revised Delayed Recall (HVLT-R DR), which showed a median decline of 0 for patients who received memantine in comparison to those in the placebo group, who had a decline of -2. The trends of all three cognitive tests for the 149 eligible patients who survived 24 weeks indicate that the memantine group produced superior results than the placebo at all points. There was no difference in patients’ PFS or OS between the treatment arms. Patients in the study included adults who had brain metastases and were categorized by recursive partitioning analysis in either class I or II with or without or surgical resection or prior radiosurger. Patients underwent standardized tests of cognitive function, which were performed at baseline, eight, 16, 24, and 52 weeks. Just 32% of patients completed the drug therapy and evaluations principally because of poorer than estimated survival and progressive disease, which led to poor compliance with the treatment protocol. Patients in both groups reported similar levels of grade 3 and 4 toxicities, including headache, fatigue, hair loss, and nausea. “We are excited to see that adding memantine to the treatment plan for brain tumor patients helps preserve their cognitive function after whole brain radiotherapy even six months after treatment,” said Nadia N. Laack, MD, coauthor of the study and a radiation oncologist at the Mayo Clinic (Rochester, MN, USA). “Our findings suggest that memantine may prevent the changes that occur in the brain following radiation therapy, impacting future treatment practices for these patients and suggest a role for further study in other patient populations receiving radiation to the brain.” Emergency Departments Seldom Perform Pregnancy Testing of Adolescents Before Exposure to Radiation
A small number of teen-aged girls undergo pregnancy testing in the hospital emergency department (ED), even when they complain of lower abdominal pain, or before they are exposed to radiation testing. These findings were presented in October 2012 at the American Academy of Pediatrics (AAP) National Conference and Exhibition in New Orleans (LA, USA). In the study, researchers reviewed US National Hospital Ambulatory Medical Care Survey data from 2000 to 2009 on female patients aged 14 to 21 who were examined in a hospital ED. Of the 77 million girls who visited an ED over the nine-year period, just 14.5 million (18.7%) were tested for pregnancy. Of the patients complaining of abdominal pain, 42.3% were tested for pregnancy, and of those receiving radiologic imaging, 21.5% were tested. Of patients exposed to radiation that could cause birth defects (such as a chest X-ray or computed tomography [CT] scans), only 27.9% received a pregnancy test. Moreover, disparities in testing were noted based on age, race, and insurance type. “We were surprised to find that pregnancy testing occurred infrequently,” said study author Monika Goyal, MD, FAAP, from the department of emergency medicine, Children’s Hospital of Philadelphia (PA, USA). “It was particularly concerning that rates of pregnancy testing were low even among females with potential reproductive health complaints or with exposure to radiation through diagnostic testing, like CT scans. These findings underscore the need to develop quality improvement interventions to increase pregnancy testing in adolescent girls in the emergency department, especially among those with higher risk of pregnancy complications.” |
ArchivesCategories
All
|

 RSS Feed
RSS Feed
